Healthcare Integration Platform: Connect EHR, Billing, HRIS and Clinical Systems
March 23, 2026A healthcare integration platform connects Epic or Oracle Cerner EHR, RCM billing systems, HRIS platforms (Workday, UKG, ADP), clinical quality reporting databases, and lab systems into a single HIPAA-compliant automated data flow, eliminating the manual reconciliation work that currently costs healthcare organisations an estimated $15.4 billion annually in physician productivity losses. eZintegrations connects the complete healthcare technology stack using FHIR R4 and HL7 v2 interfaces, 5,000+ pre-built API endpoints, and Automation Hub templates, with the first integration live in hours and no HL7 licensing fees required.
TL; DR
Physicians in disconnected healthcare systems spend nearly 50 minutes per day reconciling information across different EHR, billing, and administrative platforms. Across a mid-size health system, that is thousands of hours of clinical time consumed every month by data reconciliation rather than patient care. The Global Healthcare IT Integration Market is valued at $5.81 billion in 2025 and growing at 11.85% annually, reflecting the urgency health systems feel to close their interoperability gaps.
eZintegrations connects Epic, Oracle Cerner, Meditech, billing and RCM systems, HRIS platforms (Workday, UKG, ADP), clinical quality databases, and lab systems using FHIR R4, HL7 v2, REST APIs, and 1,000+ Automation Hub healthcare templates. HIPAA-compliant by design, with audit trails, access controls, and encryption built into every workflow. If you are evaluating healthcare integration platforms, the system connection table, the step-by-step Epic-to-billing-to-HRIS workflow, and the Automation Hub template import link are in this post.
The Problem: Disconnected Healthcare Systems and the Real Cost of Data Silos
It is 7:15 AM on a Monday. Your billing coordinator opens three browser tabs: Epic, the RCM system, and the spreadsheet she uses to reconcile the differences between them. She has done this every morning for two years.
The problem is not her process. The problem is that your Epic EHR records the patient encounter. Your RCM billing system needs the encounter data to generate the claim. But those two systems do not talk to each other in real time. So every morning, she bridges the gap manually.
One floor up, your HR operations manager is doing something similar. A clinical staff member resigned last week. The separation is recorded in Workday. But Epic still shows that provider as active. Insurance claims will continue to include that provider’s credentials until someone notices and manually updates both systems. That typically happens weeks later, during a quarterly audit.
Two floors above that, your quality reporting coordinator is compiling the quarterly HEDIS measures report. The clinical quality data lives in Epic. The population health metrics live in a separate analytics database. The HRIS data on which patients belong to which care teams lives in Workday. Assembling the report requires exporting from three systems and reconciling them in Excel. It takes four days.
This is not a description of a health system with outdated technology. This is the operational baseline for the majority of mid-size healthcare organisations in the United States. A 2025 study cited by CertifyHealth found that while 71% of U.S. hospitals can electronically access patient data from external providers, only 42% routinely use that data in clinical care. The rest bridges the gaps manually.
The financial consequence is specific. Physicians spend nearly 50 minutes per day reconciling information across different EHR systems, contributing to an estimated $15.4 billion in annual productivity losses across U.S. healthcare. That is clinical time that could be spent seeing patients, not transferring data.
The regulatory consequence is equally specific. Information-blocking violations under the 21st Century Cures Act carry penalties of up to $1 million per violation. HIPAA compliance adds $10,000-$30,000 in certification expenses for mid-sized entities for each new system connection. The cost of building and maintaining compliant point-to-point integrations, using traditional HL7 interface licensing, runs $50,000-$200,000 annually for Epic alone.
An integration layer that connects your healthcare systems once, maintains HIPAA-compliant data flows, and scales with your organisation without per-interface licensing fees is not a convenience item. It is a financial and regulatory necessity.

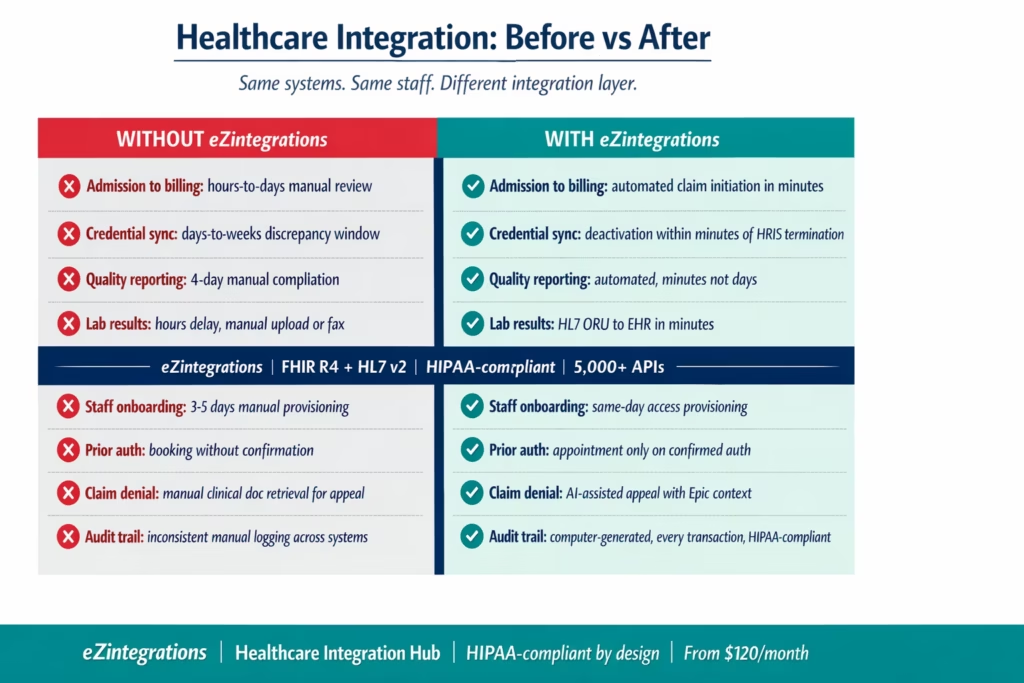
Before vs After: Fragmented Healthcare Stack vs Integrated Operations
| Dimension | Without eZintegrations | With eZintegrations |
|---|---|---|
| Patient admission to billing | ADT event in Epic triggers manual billing coordinator review. Claim generated hours to days after admission. | ADT event triggers automated claim initiation in RCM system within minutes. Billing coordinator reviews exceptions, not every encounter. |
| Provider credential sync | Provider terminated in Workday HRIS. Epic shows active for days to weeks until discovered in audit. | HRIS termination event triggers Epic credential deactivation within minutes. Zero-day window for credential discrepancy. |
| Clinical quality data to reporting | Quarterly HEDIS report assembled manually from Epic, population health database, and HRIS. 4-day compilation process. | Automated data pull from all three sources on schedule. Report compiled in minutes. Clinical quality team reviews results, not data files. |
| Lab result to EHR | Lab system generates result. Manual upload or fax to ordering provider’s EHR. Delay measured in hours. | Lab result event triggers HL7 ORU message to EHR. Result available in Epic or Cerner within minutes of lab completion. |
| Employee onboarding to clinical system access | HR onboards new clinical staff in Workday. IT manually provisions Epic access, CRM, scheduling, and clinical applications. 3-5 business days average. | HRIS onboarding event triggers automated access provisioning across all clinical systems. New staff access available same day. |
| Prior authorisation status to scheduling | Payer approves prior auth. No real-time notification to scheduling system. Patient appointment booked before auth received, generating claim denials. | Prior auth approval triggers real-time scheduling system notification. Appointments only scheduled on confirmed authorisations. |
| Claim denial to care team | Claim denied by payer. Denial sits in RCM queue. Clinical context needed for appeal must be manually retrieved from Epic. | Denial event triggers Goldfinch AI workflow: retrieves relevant clinical documentation from Epic, pre-populates appeal template, routes to appropriate care team member. |
| HIPAA audit trail | Manual compliance logging across multiple systems. Inconsistent records. Gap risk at audit. | Every integration transaction logged with timestamp, user ID, data source, destination, and outcome. Computer-generated HIPAA audit trail. |
The Six Healthcare Integration Workflows That Cost You Most
Healthcare data is not a single flow. It moves across clinical, financial, administrative, and workforce dimensions simultaneously. These six integration patterns account for the majority of manual work and compliance risk in mid-size and large health systems.
1. Epic or Cerner ADT Events to RCM Billing
Every patient admission, discharge, or transfer (ADT) event in your EHR creates a billing trigger. Without integration, your billing team monitors ADT activity manually and initiates claim generation on each encounter. With integration, the ADT event fires a webhook. The billing workflow reads the encounter details, maps to the RCM system’s claim schema, and initiates the claim automatically. The billing coordinator reviews exceptions and edge cases rather than initiating every claim from scratch.
For health systems processing hundreds of encounters per day, this integration alone reduces billing team workload by 40-60% on routine claims.
2. HRIS Provider and Staff Credential Sync to EHR
Every hire, termination, credential change, and role update in your HRIS (Workday, UKG, ADP) must be reflected in Epic or Cerner within hours, not days. The credential window, the period between an HRIS change and the corresponding EHR update, is a compliance risk. Claims submitted with terminated provider credentials trigger denials. Prescriptions from deprovisioned providers create patient safety flags.
With eZintegrations, every HRIS workflow event (new hire, termination, role change, credential update) triggers an automated update to the EHR, scheduling system, and clinical access management platform. New staff are provisioned on day one. Departing staff are deprovisioned on termination day.
3. Lab System Results to EHR via HL7 ORU
Laboratory results need to reach the ordering provider’s EHR as quickly as possible after completion. In disconnected systems, results are faxed, manually uploaded, or transmitted via a daily batch. Delays in lab result availability have direct patient safety implications and are a persistent source of physician frustration.
eZintegrations handles HL7 v2 ORU message routing from your lab information system to Epic, Cerner, Meditech, or any EHR with an HL7 v2 inbound interface. Lab completion triggers the HL7 message. The message is routed to the correct patient record and provider inbox within minutes.
4. Prior Authorisation Status to Scheduling
Scheduling a patient appointment before a required prior authorisation is received generates a denial when the claim is submitted. In a disconnected system, your scheduling team books appointments based on clinical availability without real-time visibility into the authorisation status for that patient’s procedure.
With eZintegrations, prior auth approval events from payer portals or clearinghouses trigger a real-time notification to your scheduling system. Appointments for procedures requiring prior auth are only confirmed when the authorisation is in place. Denial rates from auth-related scheduling errors drop significantly.
5. HEDIS and Clinical Quality Reporting Automation
Quarterly HEDIS measure compilation is one of the most labour-intensive recurring tasks in healthcare quality management. Data lives across Epic (clinical encounters), a population health database (patient attribution and risk stratification), and the HRIS (care team assignments). Assembling the report requires three separate exports, reconciliation, and a multi-day review process.
eZintegrations connects all three sources in a scheduled workflow. On the defined reporting schedule, the workflow queries Epic for clinical measure data, the population health platform for patient attribution, and the HRIS for care team assignments. The combined dataset is prepared and delivered to the quality team in minutes. Manual compilation is replaced by exception review.
6. Claim Denial Appeal with AI-Assisted Clinical Context
When a claim is denied, the appeal requires clinical documentation from the EHR to support the medical necessity argument. In a disconnected system, the revenue cycle team requests the clinical documentation from the clinical team, waits for retrieval, and assembles the appeal manually.
With Goldfinch AI from eZintegrations, the denial event triggers an agentic workflow: the Knowledge Base tool retrieves the relevant clinical documentation from Epic using the patient and encounter identifiers from the denial record, the Document Intelligence tool extracts the key clinical findings, and the workflow populates an appeal template with the clinical context. The appeal is routed to the appropriate clinical reviewer for sign-off before submission. The human step is review and approval, not document assembly.
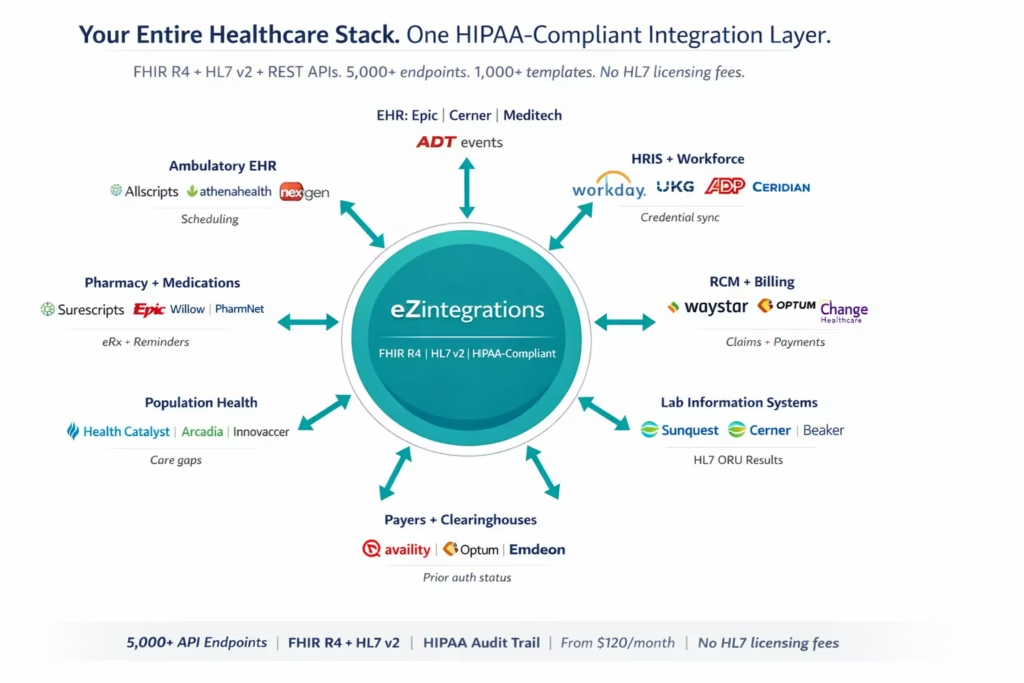
How eZintegrations Connects Your Healthcare Stack
eZintegrations connects healthcare systems via an API catalog of 5,000+ endpoints, with native support for FHIR R4, HL7 v2 message routing, and REST APIs. Every workflow includes configurable audit logging, access controls, and encryption settings that support HIPAA technical safeguard requirements.
Here is how the key healthcare system categories connect:
EHR Systems: Epic (via FHIR R4, SMART on FHIR, HL7 v2 ADT/ORU/ORM interfaces), Oracle Cerner (via Ignite APIs, FHIR R4, HL7 v2), Meditech (REST and HL7 v2), Allscripts, athenahealth, NextGen, eClinicalWorks. Patient events, clinical data, provider information, and scheduling data connect bidirectionally.
Revenue Cycle Management: Waystar (formerly Navicure/ZirMed), Optum, Change Healthcare, Epic Tapestry, Cerner RevolutionRCM, R1 RCM, athenaCollector, AdvancedMD. ADT events, claim initiation, denial management, prior auth status, and payment posting connect to clinical systems.
HRIS and Workforce: Workday HCM, UKG Pro and UKG Dimensions, ADP Workforce Now, Ceridian Dayforce, Oracle HCM Cloud, SAP SuccessFactors. Provider credentials, staff onboarding, terminations, role changes, certification updates, and schedule data connect to EHR and clinical access management systems.
Laboratory Information Systems: Sunquest LIS, Meditech LIS, Cerner PathNet, EPIC Beaker, Roper Technologies (Sunquest), Orchard Software, SCC Soft Computer, and any LIS exposing HL7 v2 ORU or REST interfaces. Lab results route to EHR provider inboxes via HL7 message delivery.
Population Health and Analytics: Health Catalyst, Arcadia, Lightbeam, Innovaccer, IBM Watson Health (Merative), Microsoft Azure Healthcare APIs. Clinical quality data, patient attribution, risk stratification, and HEDIS measure data connect to quality reporting workflows.
Payer and Clearinghouse: Availity, Optum Clearinghouse, Change Healthcare, Emdeon, ClaimMD. Prior auth status, eligibility verification, claim status, and denial data connect to clinical scheduling and RCM systems.
Pharmacy and Medication Management: Surescripts, Epic Willow, Cerner PharmNet, PioneerRx. Medication orders, dispensing events, and medication reconciliation connect to clinical workflows.
The Automation Hub provides 1,000+ pre-built healthcare integration templates. Import a template, configure your system credentials and FHIR/HL7 endpoints, validate in the Dev environment, and promote to production. Your first workflow goes live in hours. No HL7 interface licensing fees. No custom interface development.
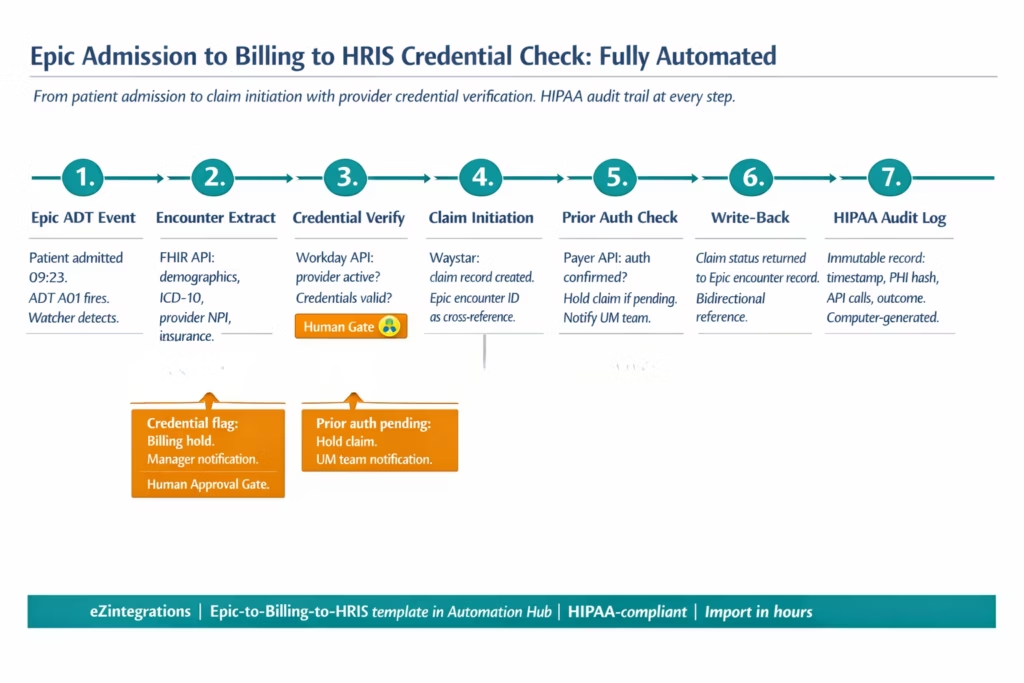
Step-by-Step: Epic ADT Event to Billing to HRIS Workforce Verification
This is the core healthcare operations integration: a patient is admitted to your facility, the clinical record is created in Epic, the billing workflow initiates automatically, and the HRIS system confirms that the assigned providers have active credentials before the claim is submitted. Every step is automated, audited, and HIPAA-compliant.
The example runs on Epic as the EHR, Waystar as the RCM system, and Workday as the HRIS. The integration runs on eZintegrations.
Step 1: Patient Admission ADT Event (HL7 v2 or FHIR Watcher) A patient is admitted at 09:23 AM. Epic generates an ADT A01 (Admit) message. The eZintegrations Watcher monitors the Epic ADT event stream (via HL7 v2 ADT interface or FHIR Encounter resource subscription). The admission event fires the billing initiation workflow.
Step 2: Encounter Data Extraction (Epic FHIR API) The workflow calls the Epic FHIR API to retrieve the full encounter record: patient demographics, admission diagnosis (ICD-10 codes), attending provider NPI, insurance information, and admitting department. This data provides the complete context needed for the billing record.
Step 3: Provider Credential Verification (Workday HRIS API) Before initiating the claim, the workflow calls the Workday API to verify: – The attending provider’s status in HRIS: active employee, active clinical credentials, no pending termination .Any credential expiry flags for the billing period . Provider’s billing NPI active and in good standing
If the provider’s HRIS status is active and credentials are valid: workflow proceeds to Step 4.
If any credential flag is raised: the workflow routes to a Human Approval Gate. The billing manager receives a notification with the specific credential issue and the patient encounter details. The claim is held until the credential discrepancy is resolved.
Step 4: Claim Initiation in RCM System (Waystar API) The workflow calls the Waystar API to initiate the billing record: patient ID, encounter ID, attending provider NPI, diagnosis codes, admission type, and insurance policy details. Waystar creates the claim record in pending status. The encounter ID from Epic is stored as the cross-reference in the claim record.
Step 5: Prior Authorisation Check (Availity or Payer API) For procedures requiring prior authorisation, the workflow queries the payer’s eligibility and authorisation API. If a prior auth is confirmed: the claim proceeds to billing. If prior auth is pending or not on file: the claim is held and a notification fires to the scheduling and utilisation management teams with the specific auth requirement.
Step 6: Claim Status Write-Back to Epic (Epic FHIR API) Waystar processes the claim and returns the claim status (accepted, pending, rejected). The workflow writes the claim status back to the corresponding Epic encounter record, creating a bidirectional reference: Epic knows the claim status, and Waystar knows the Epic encounter ID. Billing and clinical teams see the complete picture in both systems.
Step 7: HIPAA Audit Log (Immutable Transaction Record) Every step in the workflow generates an automatic, immutable audit log entry: timestamp, Epic patient ID (hashed for PHI minimisation), HRIS provider ID, Waystar claim ID, API endpoint called, data elements transmitted, and outcome status. This is the computer-generated HIPAA technical safeguard audit trail required for all electronic PHI transmissions.
Key Outcomes and Results
Healthcare integration delivers measurable outcomes across three dimensions: financial performance (revenue cycle speed and accuracy), operational efficiency (staff time and manual workload), and compliance posture (audit readiness and claim accuracy).
Billing initiation speed: Hours to minutes Transitioning from manual billing coordinator review of every ADT event to automated claim initiation on admission reduces the time from encounter to claim initiation from an average of 6-24 hours to under 5 minutes for clean encounters. For health systems with high encounter volumes, this compresses the revenue cycle and reduces days-in-AR (days in accounts receivable), directly improving cash flow.
Claim denial rate from credential errors: Reduced to near zero The primary driver of credential-related claim denials is the window between a provider change in the HRIS and the corresponding EHR update. With real-time credential sync, that window closes from days to minutes. Denials from terminated or expired provider credentials drop to near zero for health systems with integrated HRIS-to-EHR workflows.
Clinical quality report preparation: 4 days to under 30 minutes Manual HEDIS measure compilation from three separate systems typically takes 4 business days per reporting cycle. Automated data extraction and compilation reduces this to under 30 minutes for the initial dataset, with quality team time spent on review and analysis rather than data assembly.
Staff onboarding to clinical system access: 3-5 days to same day Manual provisioning of new clinical staff across Epic, scheduling systems, and clinical applications typically takes 3-5 business days. Automated HRIS-triggered provisioning delivers same-day access. For high-volume hiring periods, this reduces the backlog that delays new staff productivity.
HL7 interface licensing cost elimination Traditional HL7 interface licensing for Epic connections costs $50,000-$200,000 annually (Enter.health, 2025). eZintegrations connects to Epic via FHIR R4 and HL7 v2 interfaces without separate HL7 licensing fees, using the API catalog at flat per-automation pricing. For health systems with multiple HL7 interfaces, this represents a direct annual cost saving.
Physician reconciliation time: 50 minutes per day to near zero When clinical, billing, and administrative systems share real-time data through an integration layer, the manual reconciliation work that accounts for 50 minutes of daily physician time (CertifyHealth 2025) is replaced by exception management. Physicians address flags and discrepancies rather than routine data checking across systems.

How to Get Started
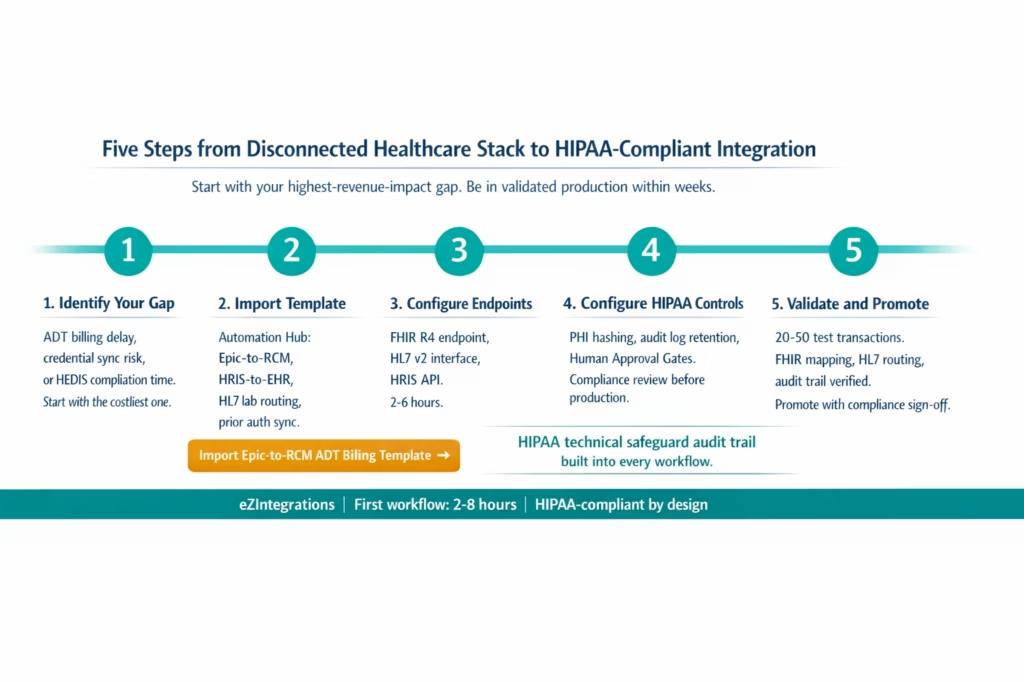
Healthcare integration has higher compliance requirements than standard enterprise integration, but the path to your first live workflow does not have to take months. Here is the five-step path from evaluation to validated production workflow.
Step 1: Identify your highest-cost integration gap Use the six-workflow framework above. Which disconnection is costing you most in billing delay, denial rates, staff time, or compliance risk? For most mid-size health systems, the highest-priority starting point is either the ADT-to-billing initiation gap (direct revenue cycle impact) or the HRIS-to-EHR credential sync gap (direct denial and compliance impact). Start with the one where the business case is clearest.
Step 2: Import the relevant Automation Hub template Go to the Automation Hub and search for your system combination. Templates are available for Epic-to-RCM ADT billing, Workday HRIS-to-Epic credential sync, lab HL7 result routing, prior auth status-to-scheduling, and HEDIS quality report compilation. Import the template for your highest-priority workflow.
Step 3: Configure FHIR or HL7 endpoints and HRIS API credentials Add your Epic FHIR R4 endpoint, HL7 v2 interface connection details, and HRIS API credentials to the eZintegrations credential vault. HIPAA-compliant credential storage with role-based access control is built into the platform. This step typically takes 2-6 hours depending on the complexity of your EHR’s interface configuration.
Step 4: Configure audit logging and HIPAA controls Enable the HIPAA audit trail configuration for your workflow: specify which data fields should be hashed (PHI minimisation), configure the audit log retention period, and set the Human Approval Gate thresholds for workflows that involve high-sensitivity clinical data transmissions. Your compliance team should review these settings before the workflow goes to production.
Step 5: Validate in Dev and promote to production Run 20-50 test transactions in the Dev environment using realistic (de-identified) data. Validate that FHIR resource mapping is correct, HL7 message routing delivers to the correct EHR provider inbox, audit logs are generated as expected, and exception notifications reach the correct staff. Document your test results. Promote to production with compliance team sign-off.
Ready to see it live? Book a free demo and bring your Epic FHIR endpoint documentation and your RCM system API credentials. We will build the ADT-to-billing workflow in the session and show you the HIPAA audit trail output.
Frequently Asked Questions
1. How do healthcare organisations use eZintegrations
Healthcare organisations use eZintegrations to connect EHR systems including Epic Oracle Cerner Meditech and athenahealth along with RCM and billing platforms HRIS systems laboratory systems population health platforms payer connections and pharmacy systems. Common integration patterns include Epic ADT events triggering billing claim initiation HRIS provider credential sync to EHR lab HL7 ORU result routing prior authorisation status updates to scheduling HEDIS data compilation and AI assisted claim denial appeals using Goldfinch AI.
2. How long does it take to set up the first healthcare integration
The first integration typically takes 2 to 8 hours of configuration time using Automation Hub templates and the no code canvas. The main time dependency is provisioning Epic FHIR R4 endpoint access which can take 1 to 5 business days depending on Epic build team involvement. HIPAA audit control configuration and compliance review also add time. Workflow setup FHIR mapping and test validation can usually be completed within a single day.
3. Does eZintegrations work with Epic Oracle Cerner and Workday
Yes. Epic connects via FHIR R4 SMART on FHIR HL7 v2 ADT ORU and ORM interfaces and Epic FHIR APIs. Oracle Cerner connects via Cerner Ignite APIs using FHIR R4 and HL7 v2 interfaces. Workday connects via REST APIs available in the eZintegrations API catalog for HRIS and credential data. Systems not in the catalog can be onboarded through self service API integration without custom development.
4. How does eZintegrations handle HIPAA compliance for healthcare integration workflows
Every integration transaction generates an immutable audit log including timestamp source and destination systems PHI fields transmitted with optional hashing execution user ID and outcome status. This provides a complete audit trail aligned with HIPAA technical safeguards. Role based access control restricts access to workflows and Human Approval Gates can be applied for sensitive clinical processes. Encryption audit logging and access control are built into the platform without requiring separate configuration.
5. Does eZintegrations eliminate HL7 interface licensing fees for Epic
Yes. eZintegrations connects to Epic using FHIR R4 SMART on FHIR APIs and standard HL7 v2 interfaces without requiring separate HL7 interface licensing fees. Traditional Epic HL7 interface licensing can cost between 50000 and 200000 dollars annually. eZintegrations uses standard interfaces and provides a fixed per automation pricing model eliminating per interface and per message licensing costs.
6. Can eZintegrations handle AI assisted claim denial appeal workflows
Yes. Goldfinch AI includes native agent tools for claim denial appeals. Document Intelligence extracts clinical data from EHR systems Knowledge Base Vector Search retrieves payer guidelines and requirements and Integration Workflow as Tool submits appeals to RCM platforms. A Human Approval Gate ensures clinical reviewer validation before submission reducing appeal preparation time from 1 to 3 days to under 2 hours for standard denial cases.
Conclusion
The data that drives better patient care and stronger financial performance exists in your health system right now. It lives in Epic, in your RCM system, in Workday, in your lab system, and in your payer connections. What it does not do, in most mid-size health systems, is flow between those systems in real time.
Physicians spend 50 minutes a day reconciling it manually. Billing coordinators bridge the gap every morning. Quality teams spend four days compiling data that could be automated in thirty minutes.
eZintegrations connects your healthcare stack via FHIR R4, HL7 v2, and REST APIs, with HIPAA-compliant audit trails, access controls, and Human Approval Gates built into every workflow. No HL7 interface licensing fees. No custom interface development. The first workflow goes live in hours.
Import the Epic-to-RCM ADT billing template from the Automation Hub and run your first test transaction today. Or book a free demo and bring your Epic FHIR endpoint documentation. We will build the workflow in the session and show you the HIPAA audit trail output.